There are many different types of herpes virus.
Additionally, you have your Zoster Virus, Epstein-barr virus associated with mononucleosis, and some lymphomas. You’ve got Cytomegalovirus, again mono-like syndrome, Roseola which is associated with Heck’s disease, and then something that more recently has been described is Kaposi sarcoma (KS) which is actually related to the presence of HHV-8.
Primary (acute) Herpetic Gingivostomatitis
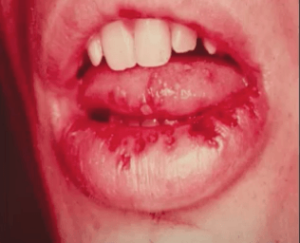
There are many different subtypes of herpes and it has a broad range of conditions associated with each specific subtype. So herpes virus infection that we’re going to talk about is primary or acute herpetic gingivostomatitis.
So this is Herpes Simplex HSV. So primary herpetic gingivostomatitis is the primary infection when you’re initially exposed to the virus.
Most people will not have this manifestation. About 12% of patients exposed to the virus are symptomatic and this is an abrupt onset with systemic symptoms.
Primary (acute) Herpetic Gingivostomatitis Symptoms
Patients will have fever chills and anorexia, be very tired, may have cervical lymphadenopathy, be in a lot of pain, oftentimes can’t eat or drink, and this is usually self-limiting. Thankfully, within two weeks the patients will feel a lot better.
Primary (acute) Herpetic Gingivostomatitis Diagnosis
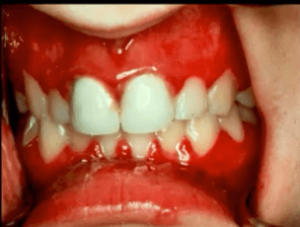
What we see orally are several tiny vesicles. This is a vesicular ulcerative condition so you’re going to see vesicles and then the vesicles will break apart and become ulcerations.
You’re also going to see diffuse involvement of the gingiva, usually they’re very swollen and very painful. The vesicles and ulcers are filled with live virus so if you touch a vesicle and then touch somebody else’s skin or your eye you can transfer herpes virus.
Herpes virus of the eye can cause blindness, so it’s very important to be self-aware of and counsel your patients so they don’t auto-inoculate others.
Oral Herpes Pictures
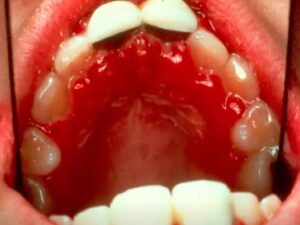
To the left is a more involved example of primary herpetic gingivostomatitis.
You’re seeing a little bit of vesicular ulcerative area around the teeth and then diffuse gingival enlargement looks almost necrotic towards the patients left rear molar. This is very painful.
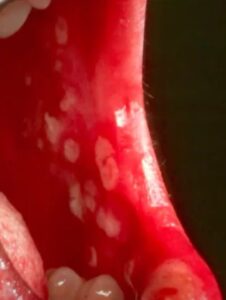
On the right are typical herpes-like ulcerations. Primary gingival herpetic gingivostomatitis can occur on moveable mucosa.
Oral Herpes Histology
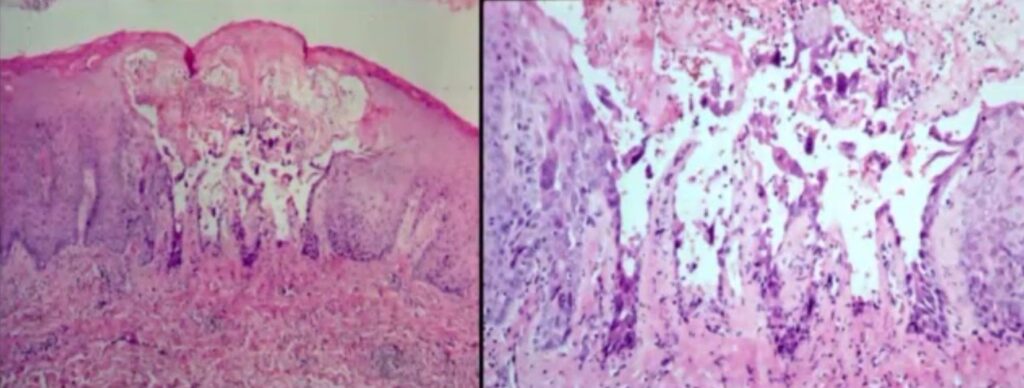
A bolus or a vesicle is a small fluid filled lesion and within the epithelium you see a small layer of parakeratin left on the top.
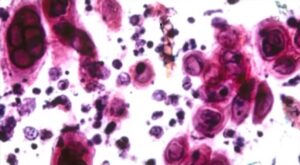
When we take a closer look into this vesicle, we see there’s some atypical cells which have a characteristic appearance when they’re infected with herpes.
There’s nuclear molding. They all mold together, and there’s chromatin pushed to the periphery so looks like an empty cell.
Oral Herpes Biopsy
When you take a biopsy and you’re not sure of herpes, if you don’t take a biopsy within the first day or so you might get a false negative. You have to biopsy the live virus. That’s what’s going after the cells. So you have to biopsy these lesions at the vesicle stage.
Diagnosis for primary herpetic gingivitis can be made clinically. The patient will have no history of herpes virus infection or anything similar to what they’re presenting and a possible contact person.
Primary (acute) Herpetic Gingivostomatitis Treatment
Caution the patient about auto-inoculation and spreading it to other people, especially the eyes. The treatment for these patients would be supportive care as far as nutrition, hydration, and NSAIDs as needed.
Don’t use aspirin.
Viscous lidocaine is OK, but make sure parents know that children should not be swallowing this because it can cause toxicity.
Resolution is usually achieved within 7-10 days. Sometimes, if you catch this early, patients will be prescribed antivirals, but usually after two or three days they have been shown that antiviral administration doesn’t have an effect on the resolution.
Other Vesicular Ulcerative Conditions
Read our previous articles on treating Pemphigus Vulgaris, understanding Erythema Multiforme and the EM-TEN Spectrum, and how to diagnose Mucous Membrane Pemphigoid.
