
Explore a variety of vesicular ulcerative conditions of the oral cavity including common conditions such as Herpes, Syphilis, Aphthous Stomatitis, and Squamous Cell Carcinomas, and rare oral diseases such as Pemphigus Vulgaris, Mucous Membrane Pemphigoid, deep fungal infections, and the EM-TEN spectrum.
Don’t have time to read the entire guide? We get it. Download the Diagnosing Vesicular Ulcerative Conditions checklist to get all the key information and images for all of the conditions covered in this article.
What’s the difference between a vesicle and an ulcer?
A vesicle is an elevated, fluid-filled lesion covered by epithelium. It is a small bulla, less than or equal to 1 centimeter in diameter. An ulcer is a defect or disruption of the epithelial component of the oral mucosa. When a vesicle loses its epithelium it presents as an ulceration.
Oral Pathology of Herpes
Primary (acute) Herpetic Gingivostomatitis
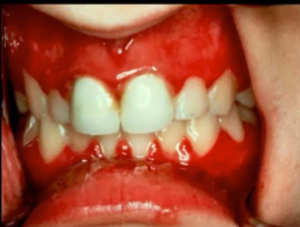
There are many different types of herpes virus; however, HSV1 and 2 are the two main types. Primary Herpetic gingivostomatitis (Herpes Simplex Virus) is the initial infection. However, most people will not have this manifestation, as only 12% of patients are symptomatic.
Patients will have fever chills and anorexia, be very tired, may have cervical lymphadenopathy, be in a lot of pain, often can’t eat or drink, and this is usually self-limiting. Mouth herpes is a vesicular ulcerative conditions so you’re going to see ulcers and vesicles (when break apart, they become ulcerations).
Treatment involves taking a biopsy of the live virus. Caution the patient about auto-inoculation, and suggest supportive care in nutrition, hydration, and supplementing NSAIDs as needed.
Secondary (Recurrent) Herpetic Eruptions
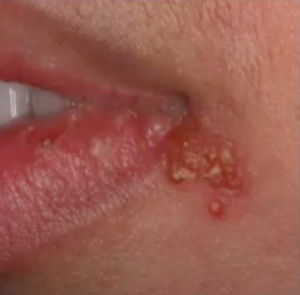
Secondary or recurrent herpes is the form with which most of us are familiar. Once the infection happens, the virus remains dormant in your trigeminal ganglion.
Herpetic eruptions appear on the skin around and inside the mouth as little vesicles, which become crusty after a few days. Intraorally, you may or may not see the blisters because of trauma.
Often, biopsies of herpes manifestations that are further along will come back with a false negative. Furthermore, doctors must consider that the patient might be immune-compromised. If you see herpes and you can only really tell by biopsying moveable mucosa, then you’ve got to start working the patient up from an immunocompromised state.
Oral Pathology of Syphilis
Primary, Secondary, and Tertiary Syphilis
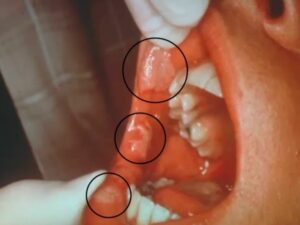
Syphilis is on the rise across the US, and there can be primary, secondary, or tertiary forms. Primary Syphilis manifests as a chancre at the site of inoculation, and frequently the chancre is on the lip. If these lesions are biopsied, they will resolve, and then the patient will go into the secondary syphilitic stage, or the virus may go dormant.
Secondary Syphilis goes from localized to disseminated, and it is usually diagnosed ten weeks after the initial infection. Both of these types incur flu-like symptoms, malaise, fever, lymphadenopathy, and maculopapular cutaneous rashes that begin on the palms and soles.
Tertiary Syphilis is much more severe, and impacts internal organs, causes aneurysms, and potentially heart failure.
Oral Pathology of Aphthous Stomatitis
Diagnosis, Treatment, and Clinical Pictures
Aphthous Stomatitis has three main subtypes: minor, major, and herpetiform aphthae. In general, an aphthous ulcer is very common; 20% of the population is affected. While there are no known triggers, it is an autoimmune disorder.
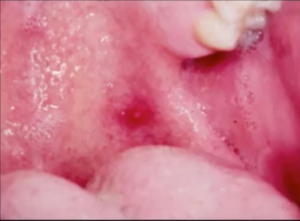
Aphthous Stomatitis is not going to be precipitated by a vesicle. It doesn’t have a vesicular stage. Once the ulcer has appeared, the active disease is over, and the treatment of the ulceration should be directed at pain relief. These ulcers can be quite large with an erythematous halo on unmovable mucosa.
For aphthous ulcers, the diagnosis is a clinical diagnosis. If you do take a biopsy of an aphthous ulcer, you won’t get a report, because it’s nonspecific. Treat aphthous ulcers with topical, systemic, intralesional corticosteroids and immunosuppressives. Herpetiform aphthae are treated with topical, systemic corticosteroids and tetracycline mouth rinse.
Aphthous Stomatitis and Crohn’s Disease
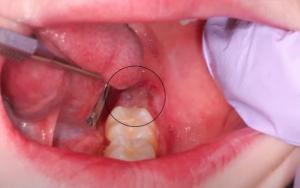
Recurrent ulcerations in the mouth can be indicative of nutritional deficiencies, blood deficiencies, and Crohn’s disease. Because there is no vesicle stage, this doesn’t fit with primary or secondary oral herpes or Aphthous Stomatitis. Dentists should ask patients if their bowel movements have changed.
If you’re not sure what it is, take a biopsy. Crohn’s diseases can manifest orally like aphthous stomatitis, but the ulcerations are usually more frequent and severe. Oral ulcers can also manifest as a generalized labial mucosae enlargement, inflammatory hyperplasia with fissuring (cobblestone effect), polypoid tag-like lesions on vestibular and retromolar mucosa, and linear ulcerations with hyperplastic margins.
Oral Pathology of Traumatic Ulcers
Traumatic Ulcerative Granuloma & TUGSE
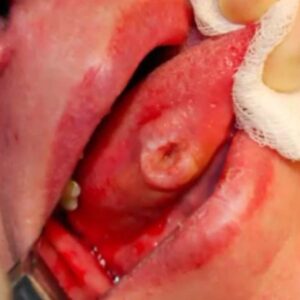
In necrosis, the tissue becomes dead. In situations where necrosis occurs, but the epithelium looks okay, you have to look at the keratinocytes. If you see keratinocytes without nuclei this tells us that the epithelium is necrotic. When the necrotic epithelium sloths, a traumatic ulcer in the mouth will form.
Traumatic Ulcerative Granuloma with Stromal Eosinophilia (TUGSE), means that there is a lot of eosinophils present. The main differential here is Squamous Cell Carcinoma.
For TUGSE, you would take a biopsy if it’s an ulcer of perilesional tissue. Once you biopsy the lesion, it starts to resolve on its own with new blood flow in the area. It is chronic, but it is self-limiting after the biopsy. Do not wait a couple of weeks to take a biopsy.
Oral Pathology of Squamous Cell Carcinoma
Oral Cavity and Oropharyngeal SCC
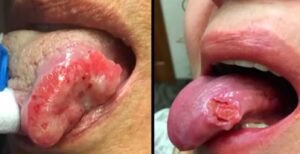
Squamous Cell Carcinoma (SCC) lesions can look similar to Traumatic Ulcerative Granuloma with Stromal Eosinophilia (TUGSE), but SCC is a bit more involved. Cells that look abnormal in shape and size and present stains with atypical mitotic activity are key indicators of Squamous Cell Carcinoma. In general, we combine the oral cavity and Oropharyngeal squamous cell carcinoma (OPSCC) statistics into one. However, it’s two separate entities.
Oropharyngeal Squamous Cell Carcinoma & HPV
The overwhelming majority (73%) of Oropharyngeal Squamous Cell Carcinomas are related to HPV, whereas the majority of Oral Cavity SCC is not associated with HPV. We know that the high-risk areas remain the same: lateral borders of the tongue, ventral tongue, the floor of the mouth, soft palate. We know that soft palate tonsillar pillars and base of tongue regions are more subject to infection with HPV and therefore are more likely to develop HPV associated carcinomas.
Squamous Cell Carcinoma Pictures
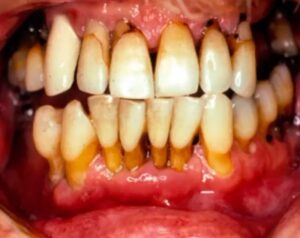
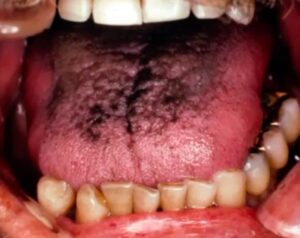
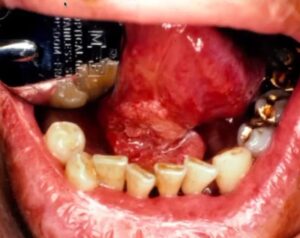
To help you identify mouth cancer, we collected clinical pictures of Squamous Cell Carcinomas affecting the gingiva, post-extraction areas, and periodontal regions.
Uncommon Ulcerations of the Oral Cavity
Oral Pathology of Pemphigus Vulgaris
Pemphigus Vulgaris is a chronic mucocutaneous vesicular bullous condition, is autoimmune, and is caused by antibodies that target the attachments between cells.
Pemphigus Vulgaris is found in the soft palate, buccal mucosa, ventral tongue, lower lip, gingiva. Crusted lesions in a variety of states of healing will be prevalent. When you have diffuse ulcerative lesions involving other areas of the body, you need to think about Pemphigus.
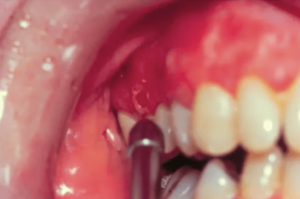
One of the clinical tests that you can do, although it might cause the patient pain, is a Nikolsky Sign, typically on a new lesion with underlying denuded connective tissue.
If you can catch and make the diagnosis early, you can potentially prevent skin lesions, which is why Pemphigus Vulgaris is something that you need to have on your radar.
Pemphigus Vulgaris can be treated systemically. In the past, they’ve frequently used steroids, but now they’re starting to use more steroid-sparing agents because there are so many complications with long-term steroid use. Good oral hygiene is also important because inflammation, plaque, and calculus can exacerbate the lesions.
Mucous Membrane Pemphigoid
Mucous Membrane Pemphigoid is a chronic autoimmune mucocutaneous vesiculobullous disease where autoantibodies target components of the basement membrane. Blistering lesions most often affect the mucous membranes of the mouth and eyes.
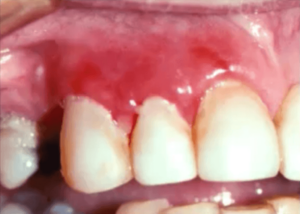
Because you’re not going to be able to tell the difference clinically if the lesions don’t resolve you’ve got to start thinking outside the box.
A lot of dentists, in general, think of gingivitis, and the first thing you might do here is clean the patient’s teeth. However, these lesions are erosive, and it is so painful for this patient to brush that they don’t brush.
If the mucous membrane of the eye is traumatized, it will heal right on top of the eyeball, or the iris, and that is called a symblepharon, a mucosal attachment to the eye. When this becomes widespread, it can cause blindness. If you ever have a patient that has been diagnosed with pemphigoid, you need to refer them to an ophthalmologist as soon as possible.
Infectious Lesions of the Oral Cavity: Histoplasmosis & Mucormycosis
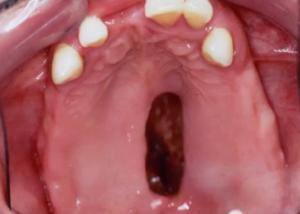
Histoplasmosis or H. capsulatum or dimorphic fungus, is the most common deep fungal infection and commonly will present in the oral cavity as an indurated ulceration.
Histoplasmosis is an infection that’s usually inhaled by spores and typically found in specific regions of the United States and other areas. There are other types of deep fungal infections namely, Blastomycosis and Coccidioidomycosis.
The diagnosis is typically made by biopsy and then confirmed by a culture or urine test. Because the microorganisms are so small, deep fungal infections can be easily overlooked. Sometimes a biopsy can reveal very sparse fungal organisms and mostly necrosis, and without a GMS stain and PAS stain, can be very difficult to see. The treatment is heavy, systemic anti-fungal agents such as Amorphotericin B or Itraconazole.
Erythema Multiforme & the EM-TEN Spectrum
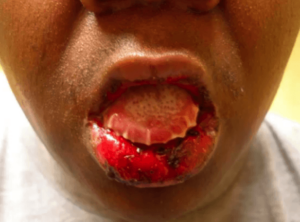
Erythema Multiforme is a mucocutaneous condition that can cause lesions of the mucous membranes and the skin, which often looks like Pemphigus Vulgaris. This is autoimmune, but it’s thought to be more of a hypersensitivity-type reaction or immune complex condition.
Typical symptoms include diffuse lip involvement, blood-crusted lips, and ulcerative lesions of the lips. Patients will have what we call target lesions or target-wide lesions oftentimes on their hands, feet, and their palmar or plantar surfaces.
Typical treatment includes systemic steroids and Valtrex 500mg once/per day.
The spectrum of Erythema Multiforme ranges from Steven-Johnson Syndrome to Toxic Epidermal Necrolysis. Steven-Johnson Syndrome is an atypical confluent of skin lesions with severe mucosal erosions involving less than 10% of the body surface. The most involved end of the spectrum is Toxic Epidermal Necrolysis when you have lesions involving more than 30% of the body surface.
Continue your Dental Education Online with a Graduate Program in Oral Pathology
Are you a lifelong learner who wants to earn while you learn? Check out our competency-based, online Oral Pathology and Radiology programs for full-time, practicing dentists.

