Discover how to image the airway obstruction site with patients suffering from Obstructive Sleep Apnea and other Sleep Breathing Disorders with Dr. Glenn Clark of the Orofacial Pain and Oral Medicine program at the Herman Ostrow School of Dentistry of USC.
Can you effectively image the site of airway obstruction?
The short answer is NO, not with any great confidence. This would be like taking a photograph of someone standing still and predicting how fast they can run. It is not an exact science and several people have tried (including me).
In the study Sites of Obstruction in Obstructive Sleep Apnea conducted by Rama AN eta, they explore various proposed sites of airway obstruction. Although there was considerable variability in the techniques and the results, the most common site of obstruction detected was at the level of the oropharynx, with extension to the laryngopharynx commonly observed.
Like what you’re learning? Take it a step further and test your clinical diagnosis skills with USC’s Virtual Patient Simulation. Review real-life patient histories, symptoms, and imaging, conduct a medical interview and clinical exam, make a diagnosis, and create a treatment plan for virtual patients experiencing Orofacial Pain conditions.
Imaging OSA with a Fast MRI
The speed of the MRI is not the issue, although faster is always better. It is the noise that occurs inside an MRI tube that is the problem. You are not sleeping when it is so loud ,and awake airways are different than sleeping airways.
Japanese author and researcher Yokoyama M, evaluated the efficacy of sleeping tubes in his study Evaluation of the pharyngeal airway in obstructive sleep apnea: a study by ultrafast MR imaging. While he claimed he could, almost every patient I have sent to an MRI says they can’t sleep in the tube.
Ultrafast MR Imaging Obstructive Sleep Apnea
- Evaluate dynamic morphologic changes of the respiratory tract in OSA
- Cross section & midline sagittal section of upper respiratory tract measured
- Using ultrafast MR imaging technique
- 10 men and 2 women diagnosed with OSA
- 30 images obtained in 30-90 s at sagittal and multilevel transverse view
- Cineloop display in awake and sleeping status
Results:
- No patients had complete pharyngeal obstruction while awake.
- 9 out of 12 had at least one occluded site during sleep.
- 3 out of 12 had multiple obstructed sites during sleep.
We are convinced that ultra-fast MR imaging is very useful in determining the indication and the method for surgical treatment for OSA.
Imaging the Airway Site of Obstruction with a CT Scan
In my study with Ogawa T, Enciso R, Evaluation of Cross-section Airway Configuration of Obstructive Sleep Apnea, we photographed obstructions of the airway. The figures below visualize this.
Fig. 1. The region of interest selected by the operator as the oropharyngeal region defined in two planes: the mid-sagittal view of the airway (a) and the axial image (b).
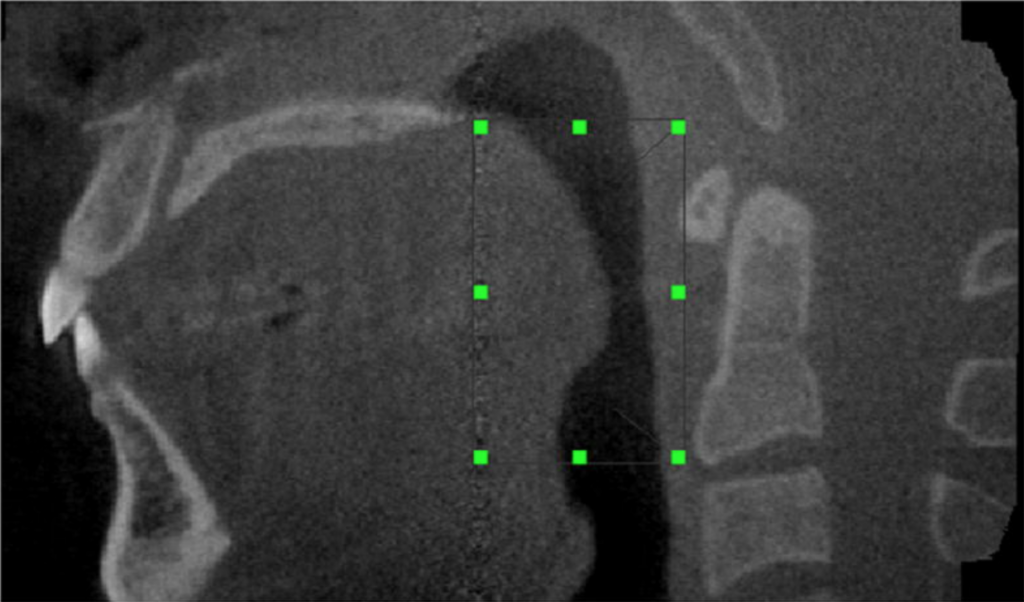
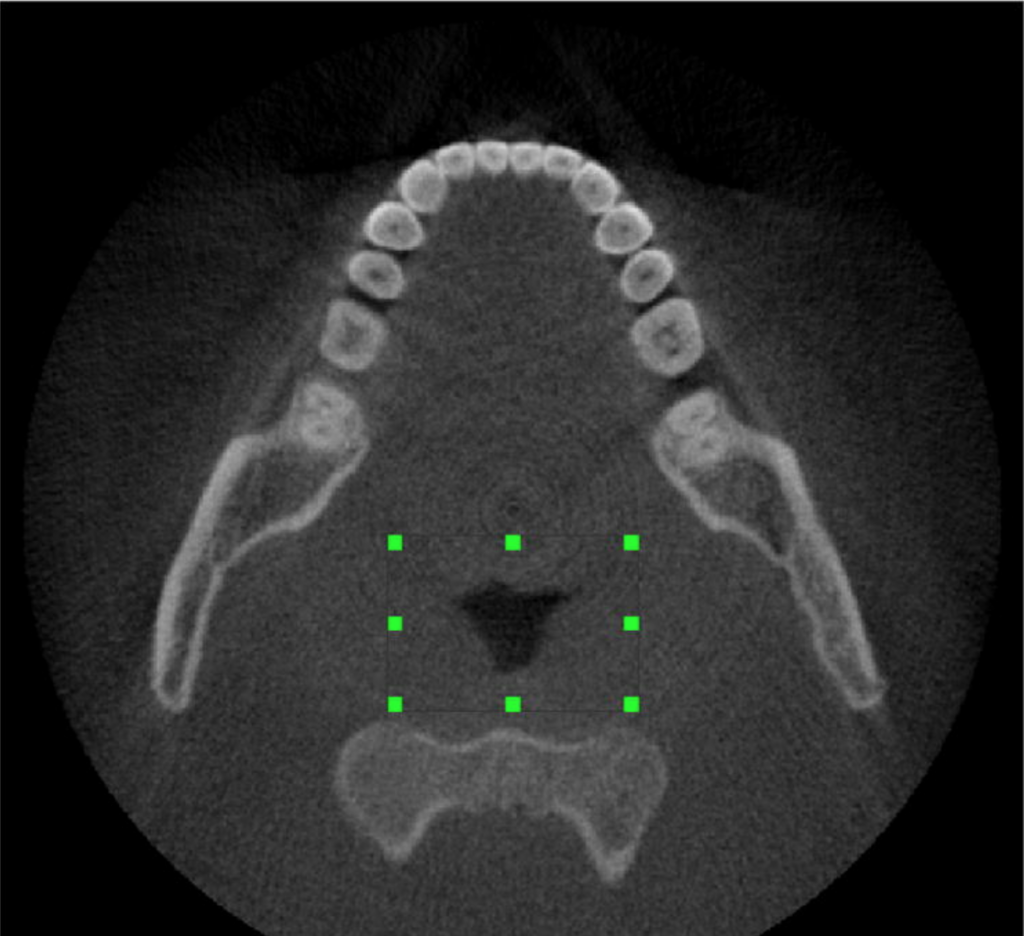
Fig. 2. Volume computed of the oropharyngeal region for a control (a and b) and an OSA case (c and d).
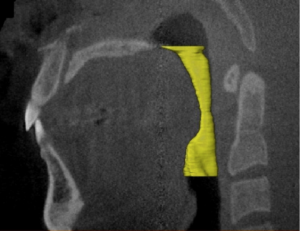
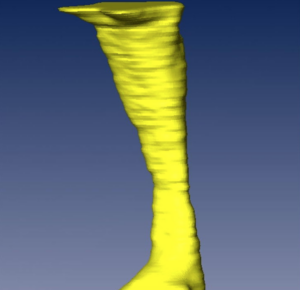
Volume computed of the oropharyngeal region for control.
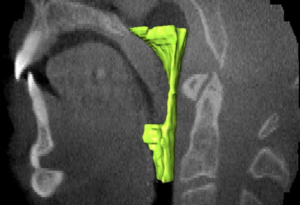
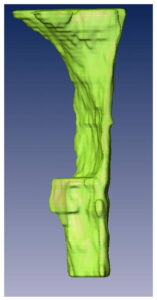
Volume computed of the oropharyngeal region for a patient with Obstructive Sleep Apnea.
Fig. 3. Axial NewTom image of the smallest cross-section area the anteroposterior (7.3 mm) and (b) lateral dimensions (17.7 mm).
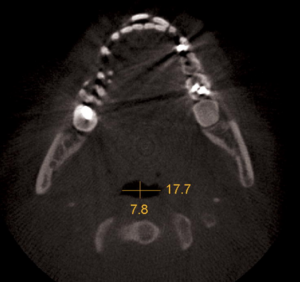
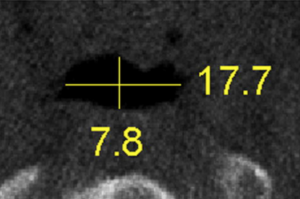
Table 1: Comparison of OSA and Non-OSA Subjects
| OSA | non-OSA |
| AP = 4.6 ± 1.2 mm L = 11.6 ± 4.5 mm Area = 45.8 ± 17.5 mm^2 AP/L = 0.39 | AP = 7.8 ± 3.31 mm L = 16.2 ± 6.8 mm Area = 146.9 ± 111.7 mm^2 AP/L = 0.48 |
Table 2: Airway Comparison of OSA vs. Non-OSA
| 1. Has your weight changed? | Increased | Decreased | No change | ||
| 2. Do you snore? | Yes | No | Do not know | ||
| 3. Snoring loudness? | Loud as breathing | Loud as talking | Louder than talking | Very loud | |
| 4. Snoring frequency? | Almost every day | 3-4 times per week | 1-2 times per week | 1-2 times per month | Never or almost never |
| 5. Does your snoring bother other people? | Yes | No | |||
| 6. If present, how often have your breathing pauses during sleep been noticed? | Almost every day | 3-4 times per week | 1-2 times per week | 1-2 times per month | Never or almost never |
| 7. Are you tired after sleeping? | Almost every day | 3-4 times per week | 1-2 times per week | 1-2 times per month | Never or almost never |
| 8. Are you tired during waketime? | Almost everyday | 3-4 times per week | 1-2 times per week | 1-2 times per month | Never or almost never |
| 9. Have you ever fallen asleep while driving? | Yes | No | |||
| 10. Do you have high blood pressure? | Yes | No | Do not know |
Conclusion:
We could generally find a difference in airway size, but these differences are lost when you match OSA and Non-OSA patients by weight and age. Most of the early studies did not have equally matched groups.
Learn Dental Sleep Medicine
Are you a lifelong learner who wants to keep practicing while you learn? Check out our competency-based, Orofacial Pain and Oral Medicine program for full-time, practicing dentists.

