Saliva, its function and benefits
Saliva provides important protection to the teeth and the tissues of the mouth due to its cleansing, lubricating and antimicrobial properties [11], [12]; promotion of remineralization of the teeth; transport of digestive enzymes; and assistance in speech, mastication and deglutition [13], [14], [15].
When the term “dry mouth” is invoked, it should be used to describe the objective finding of a decrease in the amount of saliva secreted as measured through a clinical assessment technique. Such a finding could also be called, salivary hypofunction [16].
During this clinical assessment there may also be a finding of a change in the physical composition of saliva such as its viscosity (provided mostly by mucins) – that can be evaluated by collecting samples on paper strips from different mucosal surfaces – or color (clear or cloudy) that may indicate infection or be a further indication of decreased volume [17], [18], [19].
The term “dry mouth” has also been used to describe the patient’s subjective sensation, which is correctly called “xerostomia.” Such a sensation may also be found even in patients with normal salivary gland function [20]. Studies have demonstrated that dry mouth is a common symptom. Hopcraft and Tan indicate that there is a 20% prevalence of dry mouth complaints in the general population [15].
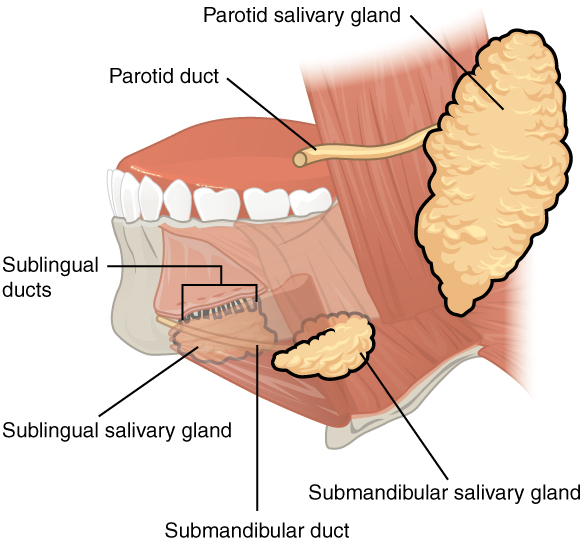
Typical saliva production has been measured at 0.5–1.5 l per day in the healthy adult [21]. Saliva is produced by three pairs of major salivary glands (parotid, submandibular and sublingual), which make a significant contribution to the overall amount of mixed saliva found in the mouth (90% by some estimates) with the remainder coming from the minor salivary glands located throughout the oral cavity on the mucosal surfaces.
Saliva is produced by acinar cells of two types: serous and mucous cells with serous cells making up the majority of the parotid gland, mucous cells making up the sublingual gland and the submandibular gland containing a combination of mucous and acinar cells [22]. For the most part the minor salivary glands are mixed glands although there are a few that are strictly mucous (palatinal glands) and some that are serous (lingual von Ebner’s glands) [23], [24].
The sympathetic and parasympathetic nervous systems are independently involved in the secretion of saliva with the fluid component including ions, responding to the parasympathetic system and a protein component responding to sympathetic stimuli [22], [25].
Control of salivary secretion is complex with the sympathetic and parasympathetic systems regulating not only the secretory function but also the reabsorption process that goes on in the striated ducts of salivary glands [26], [27].
In addition to conditioned reflexes (remember Pavlov’s dog studies), unconditioned reflexes can also stimulate salivary flow [28]. Mastication affects the salivary flow rate via periodontal mechanoreceptors and mechanical stimulation of the oral mucosa and tongue.
Postgraduate Degrees in Geriatric Dentistry
Are you looking for improved ways to diagnose, treat, and manage the oral healthcare of older patients? Explore the Herman Ostrow School of Dentistry of USC’s online master’s and certificate program in Geriatric Dentistry.
About the Authors
The article, “Dry mouth: A critical topic for older adult patients,” was authored by Phuu Han, Piedad Suarez-Durall, and Roseann Mulligan, Director Geriatric Dentistry Master and Certificate programs at the Herman Ostrow School of Dentistry of USC, and was originally published by Elsevier in the Journal of Prosthodontic Research.
References
11. A. Wolff, P.C. Fox, J.A. Ship, J.C. Atkinson, A.A. Macynski, B.J. Baum
Oral mucosal status and major salivary gland function
Oral Surg Oral Med Oral Pathol, 70 (1990), pp. 49-54
12. M. Bergdahl, J. Bergdahl
Low unstimulated salivary flow and subjective oral dryness: association with medication, anxiety, depression, and stress
J Dent Res, 79 (2000), pp. 1652-1658
13. I. Kaplan, L. Zuk-Paz, A. Wolff
Association between salivary flow rates, oral symptoms, and oral mucosal status
Oral Surg Oral Med Oral Pathol Oral Radiol Endod, 106 (2008), pp. 235-241
14. A. Chen, Y. Wai, L. Lee, S. Lake, S.B. Woo
Using the modified Schirmer test to measure mouth dryness: a preliminary study
J Am Dent Assoc, 136 (2005), pp. 164-170
15. M.S. Hopcraft, C. Tan
Xerostomia: an update for clinicians
Aust Dent J, 55 (2010), pp. 238-244
16. K. Whaley, J. Williamson, D.M. Chisholm, J. Webb, D.K. Mason, W.W. Buchanan
Sjogren’s syndrome. I. Sicca components
Q J Med, 42 (1973), pp. 279-304
17. J.J. Napeñas, M.T. Brennan, P.C. Fox
Diagnosis and treatment of xerostomia (dry mouth)
Odontology, 97 (2009), pp. 76-83
18. V. Visvanathan, P. Nix
Managing the patient presenting with xerostomia: a review
Int J Clin Pract, 64 (2010), pp. 404-407
19. R. Pramanik, S.M. Osailan, S.J. Challacombe, D. Urquhart, G.B. Proctor
Protein and mucin retention on oral mucosal surfaces in dry mouth patients
Eur J Oral Sci, 118 (2010), pp. 245-253
20. S. Furness, G. Bryan, R. McMillan, S. Birchenough, H.V. Worthington
Interventions for the management of dry mouth: non-pharmacological interventions
Cochrane Database Syst Rev, 9 (2013), CD009603s
21. S.P. Humphrey, R.T. Williamson
A review of saliva: normal composition, flow, and function
J Prosthet Dent, 85 (2001), pp. 162-169
22. H. Mese, R. Matsuo
Salivary secretion, taste and hyposalivation
J Oral Rehabil, 34 (2007), pp. 711-723
23. A.M. Pedersen, A. Bardow, S.B. Jensen, B. Nauntofte
Saliva and gastrointestinal functions of taste, mastication, swallowing and digestion
Oral Dis, 8 (2002), pp. 117-129
24. P.C. Fox, K.A. Busch, B.J. Baum
Subjective reports of xerostomia and objective measures of salivary gland performance
J Am Dent Assoc, 115 (1987), pp. 581-584
25. C. Scully
Drug effects on salivary glands: dry mouth
Oral Dis, 9 (2003), pp. 165-176
26. B.J. Baum
Neurotransmitter control of secretion
J Dent Res, 66 (1987), pp. 628-632
27. J.H. Thaysen, N.A. Thorn, I.L. Schwartz
Excretion of sodium, potassium, chloride and carbon dioxide in human parotid saliva
Am J Physiol, 178 (1954), pp. 155-159
28. M.M. Schubert, K.T. Izutsu
Iatrogenic causes of salivary gland dysfunction
J Dent Res, 66 (1987), pp. 680-688