Bruxism Definition
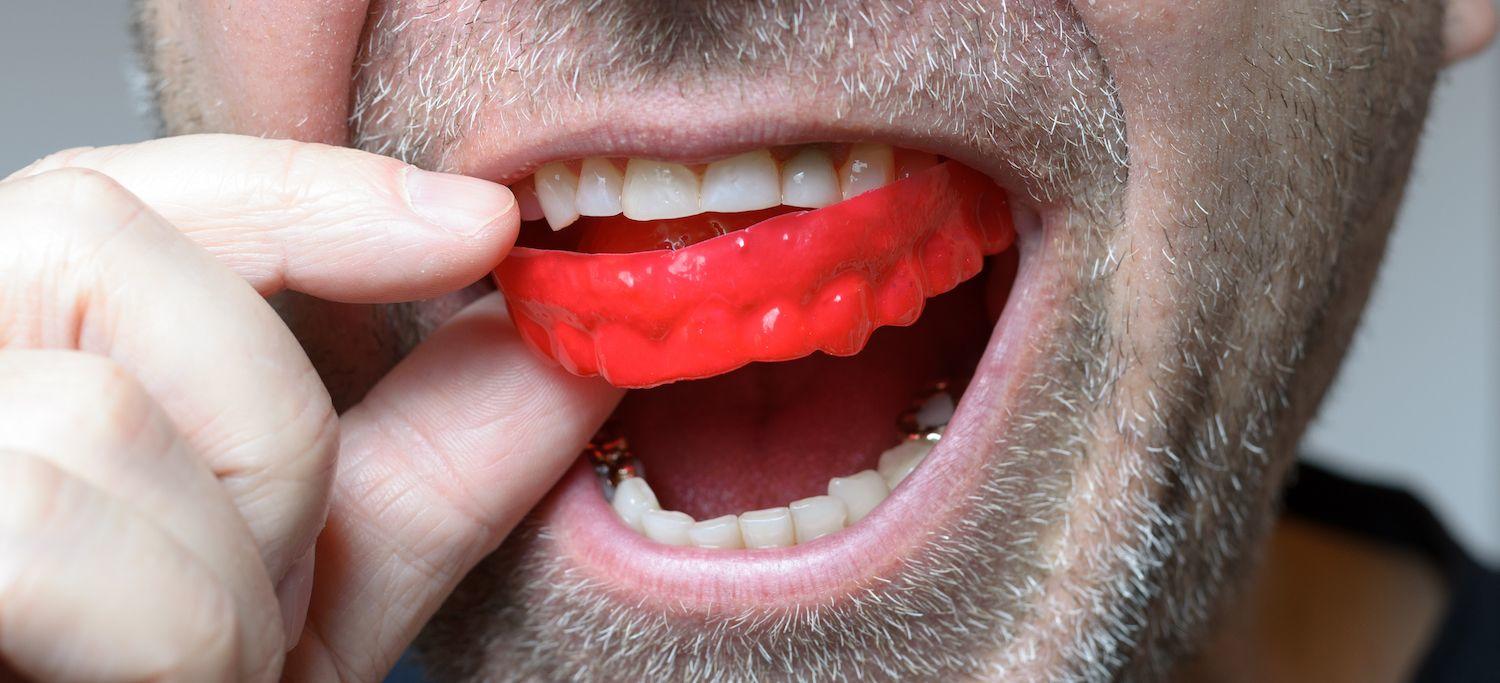
Bruxism can be defined as nonfunctional jaw movement that includes clenching, grinding, clicking, and gnashing of teeth during sleep.
Based on EMG recording of the jaw closers during sleep, there are two basic patterns of bruxism reported: (1) rhythmic, side to side motions and (2) prolonged, maximal isotonic contractions of the jaw muscles (up to 300 seconds in length). Bruxism usually occurs during sleep but with functional abnormality of the brain, can also be seen during consciousness (awake bruxism). [1]
The clinical indicators are attrition, bilaterally sore masseter and temporalis muscles, temporomandibular joint pain and jaw locking on waking. Patients are not always aware of the behavior while sleeping although they may feel the after-effects (e.g. sore jaw, sore teeth and even headaches). There is also a reported association between bruxism and otologic symptoms. [2]
Bruxism has been reported during each stage of sleep; however, the majority of episodes appear during stage II sleep and some bruxism episodes appear to be part of an arousal phenomenon, which is accompanied by an increase in heart rate and respiration. [3]
The prevalence of chronic bruxism is unknown; since no large probability-based random sample study has been performed using polysomnography (which is needed to measure bruxism). Based on a combination of attrition assessment and reports by parents, spouse or roommates it is estimated that 5 to 37% of the population has noticeable sleep bruxism. [4]
Unfortunately, many bruxers do not have substantial tooth attrition even though they clench and grind their teeth with substantial force. Also, many bruxers do not make tooth grinding sounds during sleep so examining the teeth or asking a sleep partner or parent about grinding sounds is not always an accurate way to determine its presence.
Like what you’re learning? Test your diagnosis skills with USC’s Virtual Patient Simulation. Review real-life patient histories, conduct medical interviews and exams, make a diagnosis, and create a treatment plan for patients experiencing orofacial pain.
Proposed Mechanism
The pathophysiology of bruxism is unknown but has been related with endogenous factors (such as neuromotor dysregulation and changes in the basal ganglia), and exogenous situations, including stress and anxiety. [5] Psychological stress is considered a risk factor to develop bruxism and a predictor of temporomandibular pain. [6]
The most cogent theory describes bruxism as a neuromotor dysregulation disorder. This theory proposes that bruxism occurs due to the failure to inhibit jaw motor activity during a sleep state arousal. Palinkas et al (2017) reported that patients with sleep disorders seem to have more non-REM microarousals, suggesting an irregular sleep structure in bruxers. [7]
Additional to sleep fragmentation, bruxism has been related with medical comorbidities, such as obstructive sleep apnea and epilepsy. [8] Numerous clear-cut neuromotor diseases exhibit bruxism as a feature of the disease (e.g., cerebral palsy). The disorder of periodic limb movements or restless leg syndrome is quite similar to bruxism in timing and pattern except that it occurs in the leg muscles rather than in the jaw. [9]
Related Reading: Obstructive Sleep Apnea Questionnaires for Dentists
Many patients that exhibit headaches, jaw aches and toothache are not due to classic bruxism but due to a sustained habitual forceful clenching of the teeth (day or night). [10] [11] Unfortunately, very little data is available which examines the habitual motor patterns during the day.
5 Ways to Treat Bruxism

The treatment for bruxism includes different modalities, such as behavioral techniques, intraoral devices, medications (including botulinum neurotoxin type A), and counter stimulation. [12]
1. Behavioral Techniques
Considering the multifactorial etiology of bruxism, the reduction of risk factors is a logical approach, and frequently this requires behavioral techniques. Biofeedback therapy is effective inducing changes in several parafunctional behaviors and motor training, for example improving balance in patients with Parkinson’s disease, but there is not strong evidence that it will reduce bruxism. [13] [14]
2. Occlusal Appliance
If sleep bruxism is present, the single most effective way to protect the teeth from this behavior is to recommend that the patient have a full arch, well adjusted, and balanced contact pattern occlusal appliance fabricated for use at night. [15] [16] [17]
The problem with an occlusal covering appliance is that they do little or nothing to actually stop the bruxism and many bruxism patients wearing splints will still have headaches and bruxism-induced TMJ derangement and/or arthritis may result overtime even with nightly splint usage. [18] Nevertheless, these appliances protect the teeth from progressive attrition, fracture or mitigate clenching-induced-pulpitis.
Related Reading: How to Conduct an Endo Ice Test to Prove Irreversible Pulpitis
3. Medications
In cases where the sleep bruxism disorder is very severe and the damaging consequences are well beyond the teeth, one option is to try to suppress motor activity with medications such as clonazepam. [19]
Another promising drug is tiagabine (GabitrilTM), a GABA reuptake inhibitor that is used as an adjunctive anticonvulsant treatment of partial seizures can be helpful in bruxism reduction. [20] The doses for tiagabine used to suppress nocturnal bruxism at bedtime (4-16 mg) are lower than those used to treat seizures.
A low dose of pergolide (a dopamine modulating drug) has been reported to be effective for the suppression of severe bruxism. [21]
Bromocriptine, another dopamine agonist, has also been used to suppress bruxism. In a follow–up study on seven severe bruxers using bromocriptine, there was no significant reduction in bruxism episodes. [22]
Amitriptyline, a tricyclic antidepressant, has been shown to have no significant effect on bruxism. [23]
4. Botulinum Neurotoxin Type A (BoNT-A)
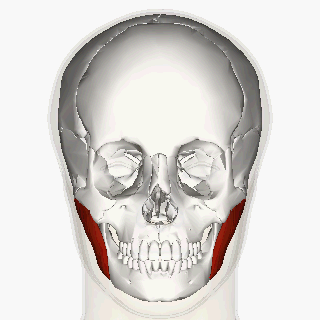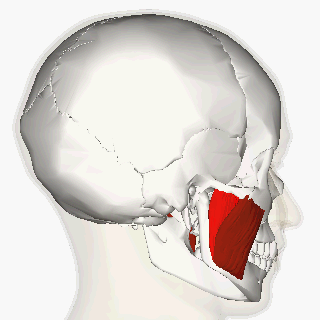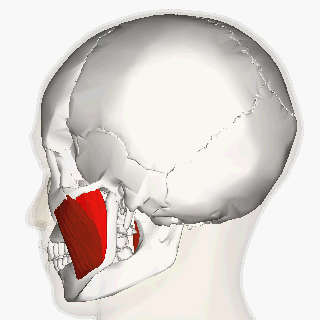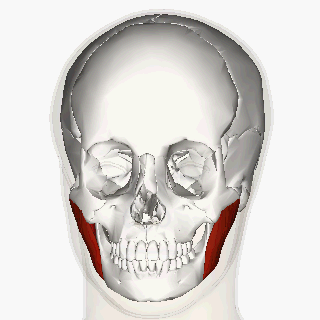
Certain patients with severe bruxism may benefit from injection of botulinum neurotoxin type A (BoNT-A) into the masseter and/or temporalis about every 3-6 months in order to minimize the power of the bruxism activity.
Unfortunately, the literature on the use of BoNT-A for bruxism is strictly case report based and has been applied mostly on brain-damaged patients who were in a comatose state. [24] [25]
The typical dosage of BoNT-A used to suppress masseter muscle activity in severe bruxism is between 60 and 65 units in the masseter per side. Potential complications include dysphagia.
For bruxism, there is no impressive data in the literature that suggests a medication (other than BoNT-A injections) can reliably suppress bruxism for more than a few days.
Behavioral approaches should be also addressed by the appropriate health care provider and will offer some help with those patients that are having an acute stress problem, which is influencing bruxism and tooth clenching behavior, but again, data on true suppression of bruxism with a behavioral approach is lacking.
5. Counter Stimulation
The use of counter stimulation (such as a small electrical impulse) activated by clenching has shown a reduction in the number and duration of bruxism events. There are several techniques for this procedure, including stimulation to the lip, masseter and temporalis muscle. [26] [27]
The use of a contingent electrical stimulation activated by clenching seems to produce a significant inhibition in the anterior temporalis muscle activity, but there is not enough evidence to suggest that this type of therapy will reduce muscle pain or jaw function. [28]
Earn a Postgraduate Degree in Orofacial Pain and Oral Medicine
Do you want to deliver appropriate and safe care to your growing and aging dental patients? Consider enrolling in our online, competency-based certificate and Master’s programs in Orofacial Pain and Oral Medicine.
References
[1] Manfredini, D., Ahlberg, J., Winocur, E., & Lobbezoo, F. (2015). Management of sleep bruxism in adults: A qualitative systematic literature review. Journal of Oral Rehabilitation,42(11), 862-874.
[2] Magalhães, B., Freitas, J., Barbosa, A., Gueiros, M., Gomes, S., Rosenblatt, A., & Júnior, A. (2017). Temporomandibular disorder: Otologic implications and its relationship to sleep bruxism. Brazilian Journal of Otorhinolaryngology., Brazilian journal of otorhinolaryngology. 2017.
[3] Ikeda, T. Nishigawa, K., Kondo K. and Clark GT. “Criteria for the Detection of Sleep Associated Bruxism in Humans” J. Orofacial Pain, 10:270-82, 1996.
[4] Khoury, S., Carra, M. C., Huynh, N., Montplaisir, J., & Lavigne, G. J. (2016). Sleep Bruxism-Tooth Grinding Prevalence, Characteristics and Familial Aggregation: A Large Cross-Sectional Survey and Polysomnographic Validation. Sleep, 39(11), 2049–2056. http://doi.org.libproxy2.usc.edu/10.5665/sleep.6242
[5] Trindade, M., Orestes-Cardoso, S., & De Siqueira, T. (2015). Interdisciplinary treatment of bruxism with an occlusal splint and cognitive behavioral therapy. General Dentistry., 63(5), E1-E4.
[6] Muzalev, K., Visscher, C., Koutris, M., & Lobbezoo, F. (2018). Long-term variability of sleep bruxism and psychological stress in patients with jaw-muscle pain: Report of two longitudinal clinical cases. Journal of Oral Rehabilitation, 45(2), 104-109.
[7] Palinkas, Marcelo, Semprini, Marisa, Filho, João Espir, De Luca Canto, Graziela, Regalo, Isabela Hallak, Bataglion, César, Rodriguez, Lais Mendes, Selma Regalo, Simone Cecilio Hallak. (2017). Nocturnal sleep architecture is altered by sleep bruxism. Archives of Oral Biology., 81, 56-60.
[8] Mayer, P., Heinzer, R., & Lavigne, G. (2016). Sleep Bruxism in Respiratory Medicine Practice. Chest., 149(1), 262-271.
[9] Malhotra, R. (2018). Neurodegenerative Disorders and Sleep. Sleep Medicine Clinics., 13(1), 63-70.
[10] Van Selms MK, Lobbezoo F, Wicks DJ, Hamburger HL, Naeije M. Craniomandibular pain, oral parafunctions, and psychological stress in a longitudinal case study. J Oral Rehabil. 2004 Aug;31(8):738-45.
[11] Takeuchi, T., Arima, T., Ernberg, M., Yamaguchi, T., Ohata, N., & Svensson, P. (2015). Symptoms and physiological responses to prolonged, repeated, low-level tooth clenching in humans. Headache : The Journal of Head and Face Pain., 55(3), 381-394.
[12] Guaita, M., & Högl, B. (2016). Current Treatments of Bruxism. Current Treatment Options in Neurology, 18(2), 10.
[13] Ilovar, S., Zolger, D., Castrillon, E., Car, J., & Huckvale, K. (2014). Biofeedback for treatment of awake and sleep bruxism in adults: Systematic review protocol. Systematic Reviews., 3, 42.
[14] Lee, B., Fung, A., & Thrasher, T. (2018). The Effects of Coding Schemes on Vibrotactile Biofeedback for Dynamic Balance Training in Parkinson’s Disease and Healthy Elderly Individuals. IEEE Transactions on Neural Systems and Rehabilitation Engineering a Publication of the IEEE Engineering in Medicine and Biology Society., 26(1), 153-160.
[15] Clark GT, Minakuchi H. The Role of Oral Appliances in the Management of TMDs. In, D. Laskin, C Green, W. Hylander, eds. Temporomandibular Disorders: An Evidenced Approach to Diagnosis and Treatment. Chicago, Quintessence Publishing Co, Inc; 2006, pp 1-15.
[16] van der Zaag J, Lobbezoo F, Wicks DJ, Visscher CM, Hamburger HL, Naeije M. Controlled assessment of the efficacy of occlusal stabilization splints on sleep bruxism. J Orofac Pain. 19(2):151-8, 2005.
[17] Macedo, C., Silva, A., Machado, M., Saconato, H., & Prado, G. (2007). Occlusal splints for treating sleep bruxism (tooth grinding). The Cochrane Database of Systematic Reviews., (4), CD005514.
[18] Can oral appliances reduce sleep bruxism?: Oral appliances for managing sleep bruxism in adults: A systematic review from 2007 to 2017. (2018). British Dental Journal : Official Journal of the British Dental Association : BDJ Online., 224(2), 80.
[19] Saletu A, Parapatics S, Saletu B, Anderer P, Prause W, Putz H, Adelbauer J, Saletu Zyhlarz GM. On the pharmacotherapy of sleep bruxism: placebo-controlled polysomnographic and psychometric studies with clonazepam. Neuropsychobiology. 2005;51(4):214-25.
[20] Kast RE. Tiagabine may reduce bruxism and associated temporomandibular joint pain. Anesth Prog. 52(3):102-4, 2005.
[21] Van der Zaag J, Lobbezoo F, Van der Avoort PG, Wicks DJ, Hamburger HL, Naeije M. Effects of pergolide on severe sleep bruxism in a patient experiencing oral implant failure. J Oral Rehabil. 2007 May;34(5):317-22.
[22] Lavigne GJ, Soucy JP, Lobbezoo F, Manzini C, Blanchet PJ, Montplaisir JY. Double blind, crossover, placebo-controlled trial of bromocriptine in patients with sleep bruxism. Clin Neuropharmacol. 2001 May-Jun;24(3):145-9.
[23] Raigrodski AJ, Christensen LV, Mohamed SE, Gardiner DM. The effect of four-week administration of amitriptyline on sleep bruxism. A double-blind crossover clinical study. Cranio. 2001 Jan;19(1):21-5.
[24] Tan EK, Jankovic J. Treating severe bruxism with botulinum toxin. J Am Dent Assoc 2000 Feb;131(2):211-6.
[25] Pidcock FS, Wise JM, Christensen JR. Treatment of severe post-traumatic bruxism with botulinum toxin-A: case report. J Oral Maxillofac Surg 2002 Jan;60(1):115-7.
[26] Nishigawa, K., Kondo, K., Takeuchi, H., & Clark, G. (2003). Contingent electrical lip stimulation for sleep bruxism: A pilot study. The Journal of Prosthetic Dentistry., 89(4), 412-417.
[27] Sumiya, M., Mizumori, T., Kobayashi, Y., Inano, S., & Yatani, H. (2014). Suppression of sleep bruxism: Effect of electrical stimulation of the masseter muscle triggered by heart rate elevation. The International Journal of Prosthodontics., 27(1), 80-86.
[28] Jadidi, F., Castrillon, E., Nielsen, P., Baad-Hansen, L., & Svensson, P. (2013). Effect of contingent electrical stimulation on jaw muscle activity during sleep: A pilot study with a randomized controlled trial design. Acta Odontologica Scandinavica., 71(5), 1050-1062.