Oral Cryotherapy
Oral cryotherapy is a very safe, easy to perform, and relatively inexpensive treatment for various selected oral lesions. You should never perform cryotherapy unless you know the diagnosis of the lesion you to freeze.
HPV is associated with papillary and verrucous lesions of skin and mucous membranes. HPV types 16 and 18 considered high risk viruses and have been identified in many oral precancerous dysplastic and squamous carcinoma tissues.
Related Reading: How to Conduct an Endo-Ice Test to Prove Irreversible Pulpitis
Don’t have time to read the entire article? Download the Endo-Ice Test Checklist for a consolidated breakdown and a brief recap of cold vs. heat vs. electric pulp testing.
Advantages of Cryotherapy
- Relatively inexpensive
- The operator does not require any skill level
- Can be performed without local anesthesia
- Extremely quick (set up and procedure)
- Useful modality for people in whom surgery is contraindicated (e.g. age, on anticoagulants, with pacemaker, allergic to anesthesia)
One disadvantage of oral cryotherapy is there is no standardization or guidelines for the delivery method and application duration.
Related Reading: How to Perform an Oral Cyst Aspiration and Cytologic Smear
Types and Methods for Oral Cryotherapy
- Liquid nitrogen Cryogen (-196°C)
- Nitrous oxide Cryogen (-88°C)
- Carbon dioxide Cryogen (-57°C)
Liquid nitrogen is useful for small lesions and can achieve more profound depth of freezing. If nerve damage occurs, it may cause taste change due to direct exposure to intraoral tissues.
Related Reading: How to Administer a Gingival Cold Test
Indications for Oral Cryotherapy
- Superficial growth of the gingival or mucosal tissues
- Actinic cheilitis
- Fibroma
- Papillomas (HPV)
- Oral leukoplakia
- Excessively pigmented lesion (e.g. hyperpigmentation or hemangioma)
Contraindications for Oral Cryotherapy
- Lesion for which histopathology is required
- Lesion is located in an area with compromised circulation
- Melanoma or any malignancy possibilities
- Patient has sensitivity or adverse reaction to cryosurgery
In general, be cautious with children because of pain complaints.
Adverse Effects & Potential Complications
Although there are minimal complications with oral lesions treated with cryotherapy, the following complications have been reported:
Short-term Effects
- Erythema and edema
- Pain during and after treatment
- Induction of headache
- Blister formation
- Secondary infection and Hemorrhage (very uncommon)
- Pyogenic granuloma
Long-term Effects
- Scar formation
- Pigmentation (Hyperpigmentation, Hypopigmentation)
- Local neuropathy
- Recurrence of the lesion
Like what you’re learning? Download a brochure for our online, postgraduate Orofacial Pain and Oral Medicine degree program.
Step-by-Step Oral Cryotherapy Procedure
1. Prepare the Cryogen
- Decant the cryogen from the storage container to the flask
- Flask should be filled from 33% to 70% for adequate function
- After the flask is filled, wait 30-60 seconds before replacing the top to allow the Cryogen to stop boiling
- Check that the rubber gasket is still in place to ensure the seal is maintained
If the cryogun has been used before, depressurize the flask before the top is removed. This can be achieved by untightening the top by a quarter to one half a turn to allow the gas to vent from the cover.
2. Select the Appropriate Tips
- Only use manufacturer’s tip.
- Tighten tip using only finger tight firmness.
3. Administer Anesthesia
Apply topical anesthesia (or sometimes local anesthesia) as needed. Consideration should be taken especially for children.
4. Administer Cryotherapy
- Ensure the unit is kept as upright as possible to prevent purging of cryogen.
- Keep the cryotip about 1-1.5 cm away from the lesion and aimed at the center of the target lesion.
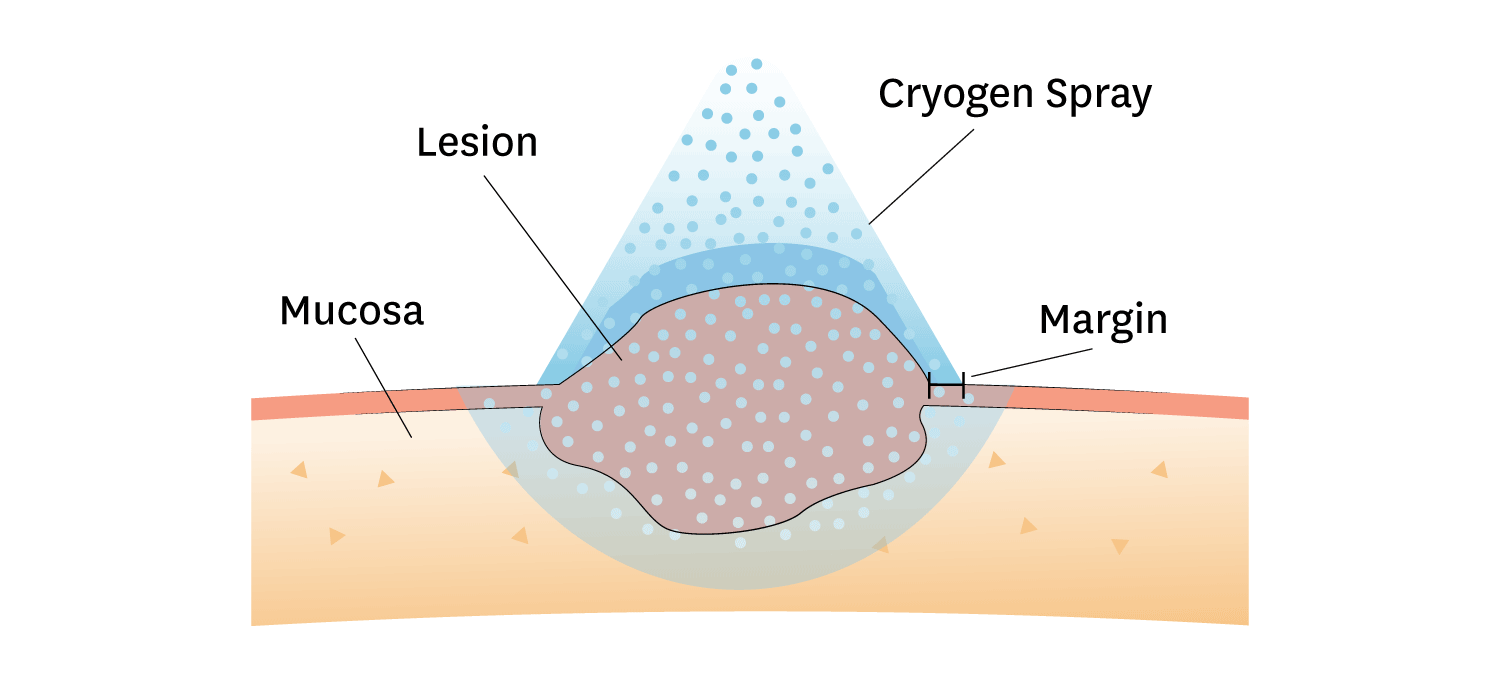
- Spray cryogen until an ice field encompasses the lesion and the desired margin (usually the Cryogen is applied for between 3-5 seconds until the light frost appears)
- Freezing should be performed until a 1-2 mm rim of frost appears around the lesion.
- If needed, a longer duration should be applied for pre-malignant lesions (e.g. leukoplakia, actinic cheilitis).
Margins
A 2-3 mm margin is required for premalignant lesions and a 5 mm margin is required for malignant lesions. Once the ice field has filled the specified margin, the spray needs to be maintained for an adequate time (between 5-30 seconds) to keep the target field frozen. However, never apply continuous freezing at one location for more than 30 seconds as this may produce scarring.
5. Repeat Freeze-Thaw Cycle
More than one freeze-thaw cycle is required, complete thawing (usually 2-3 minutes) should be allowed before the next cycle. Depending on the size and thickness of the lesion, repeat the application up to 4 times.
6. Chart the Lesions
Chart carefully all lesions that are treated and include the length of time the probe was applied in total, and the equipment used.
7. Provide Post-operative Care Instructions
For pain, patients may take Acetaminophen. If a skin blister develops it is best to leave it alone to dry up. If the blister is large, it can be pricked with a sterile needle and drained. Pigmentation changes are common in the treated site, and sometimes numbness can develop. Lastly, for multiple site involvement, repeat the same treatment for other lesions in 2-4 week intervals.
Earn a Master’s Degree in Orofacial Pain and Oral Medicine Online
Like what you’re learning? Consider enrolling in the Herman Ostrow School of Dentistry of USC’s online, competency-based 1-year certificate program or 3-year Master’s program in Orofacial Pain and Oral Medicine.


