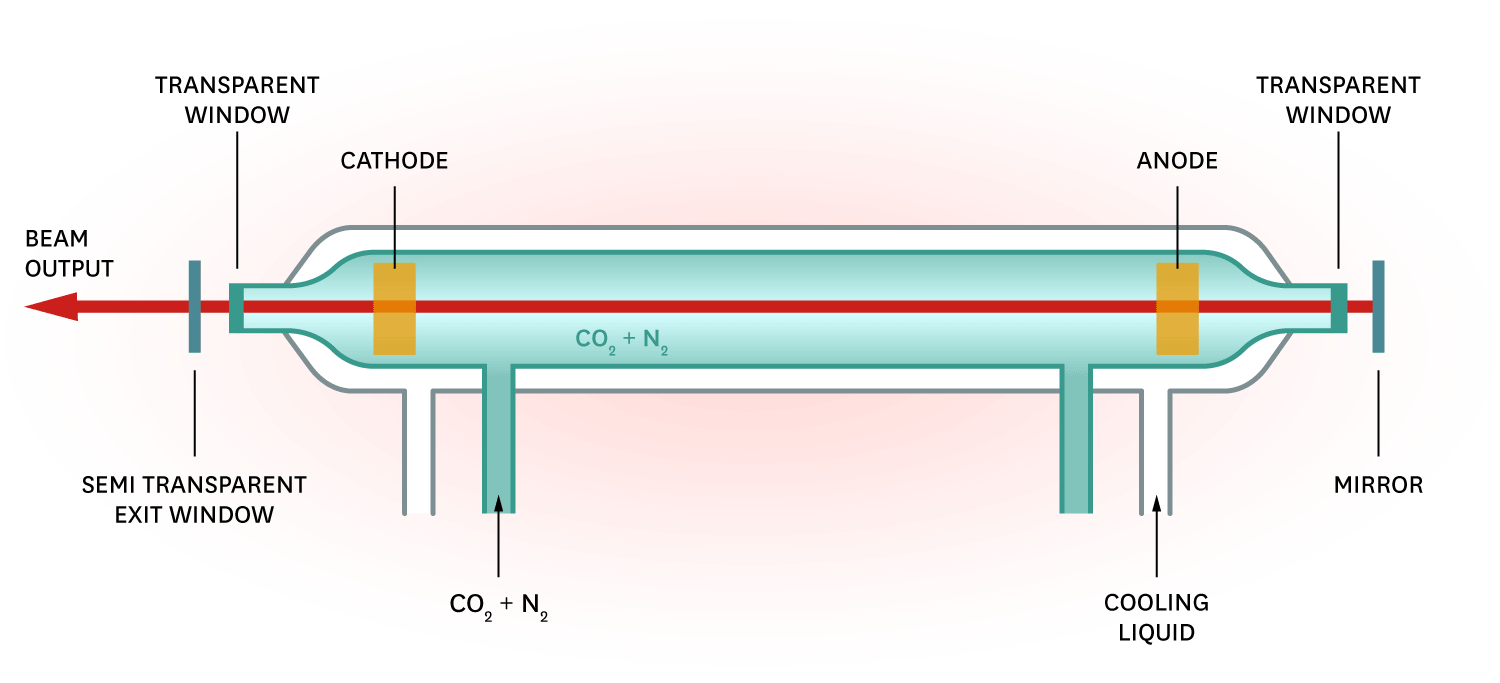
What is a laser?
Lasers are an intense, high energy, coherent (travels in a constant phase in time and space), monochromatic (a single wavelength particular to the medium), and collimated (travels in the same direction) electromagnetic radiation that is produced by a medium (solid, liquid, free particle, or gas). More simply, LASER is an acronym that stands for Light Amplification by Stimulated Emission of Radiation.
What types of lasers are used in the medical field?
Lasers that are commonly used in the medical field include:
- CO2 laser
- Er:YAG (erbium: yttrium-aluminum-garnet)
- Nd:YAG (neodymium: yttrium-aluminum-garnet)
- Argon laser
- Diode laser
- Dye laser
- Excimer laser
- Q-switched Ruby
- Q-switched Nd:YAG
Most common surgical lasers emit wavelengths in the infrared part of the spectrum:
- Nd:YAG of λ=1064 nm
- Er:YAG of λ=2.94 μm
- CO2 laser of λ=10.6 and 9.6 μm.
Within the visible portion of the electromagnetic spectrum, argon lasers emit a light between 458-515 nm, and excimer lasers emit a light in the ultraviolet part of the spectrum (100-400nm).
Like what you’re learning? Download a brochure for our online, postgraduate Orofacial Pain and Oral Medicine degree program.
How does a laser work to ablate tissues?
Lasers for ablative laser treatments interact with the tissue as photochemical interactions, photothermal effects, photoablation, plasma-induced ablation, and photodisruption. The specific interaction depends on the power, power density, energy, pulses, frequency, exposure time, focal spot size, wavelength of the laser, and tissue consistency.
1. Photochemical Interaction
Photochemical interaction occurs when using lasers with low power density and long exposure time where the laser induces a chemical effect and production of molecules in the tissues. This phenomenon is used in photodynamic therapy, where a photosensitizer is injected into the body and activated after laser irradiation.
2. Photothermal Effect
Photothermal effect is used most commonly. Depending on the power density used, this creates different tissue reactions such as coagulation, vaporization, carbonization, and melting.
Coagulation is dependent on wavelength of the laser used and has a large clinical usage on sealing blood vessels at the wound margins.
Vaporization is where the water inside the cells evaporates, with vacuole formation, cratering, and tissue shrinkage.
Carbonization occurs when the temperature increases or the power applied is too high, and carbon, gas and smoke is created which causes the color change of the tissue.
Melting is an effect where the high-energy light density “breakdown” the tissue. This effect allows you to melt the surface of a tooth or an implant in a short time.
3. Photoablation
Photoablation differs from melting where it breaks down the binding chains between the molecules rapidly and destroys the tissues. This makes precise ablation of the tissue without any evidence of thermal damage such as coagulation or vaporization.
4. Plasma-Induced Ablation
Plasma-induced ablation involves removal of tissue without thermal or mechanical damage by ablating the tissues by ionizing plasma formation. This effect has not been applied in the dental field.
5. Photodisruption
Photodisruption is a combination of plasma formation, shock wave generation, cavitation and jet formation by using higher pulse energies and pulse durations. Photodisruption is used to split tissues as in lithotripsy and lens capsulotomy.
6 Advantages and Indications for Oral Laser Ablation Surgery
- Operations usually take a short time because of the excellent visibility from bleeding control.
- More precise than standard surgical tools with less damage to normal tissues.
- Processes of wound healing are excellent because of the limited scarring and contraction.
- Useful for benign tumors (fibroma, adenoma, lipoma), pigmented lesions, drug-induced gingival overgrowth, and leukoplakia.
- Can be used for both incisional and excisional biopsy: always make a 0.5 mm margin between the cut and tissue sample and inform the pathologist for possible structural changes.
- May be a great value in managing the wound left by standard surgical tools (scalpel).
5 Disadvantages & Contraindications for Oral Ablative Laser Treatment
- Excisional biopsy for a malignant lesion is contraindicated as the pathological interpretation of laser margins will become difficult.
- Papilloma should be removed with caution as an active virus can be engulfed in the laser plume and create a new lesion in a different area. High volume suction is required to reduce the plumes as the virus may aerosolize and spread.
- Surgeons and staff/assistants must undergo a specific training and strict safety precautions must be followed.
- It is an expensive treatment and requires bulky equipment.
- The effects may not last long and you may have to repeat the treatment to get the full benefit.
Like what you’re learning? Download a brochure for our online, postgraduate Orofacial Pain and Oral Medicine degree program.
How to Perform Oral Laser Treatment
Two different techniques can be used to treat soft-tissue lesions: excision and ablation. Because the surface of most oral tissues has a high water content, CO2 laser is indicated in most cases.
1. Set Up the Equipment
Set up the laser equipment as instructed and keep the laser on “Standby mode”. Be gentle with the fiber optic cable when setting up and disassembling the unit to ensure longevity of this expensive equipment. Damaged cables will prevent proper use and render the laser useless until replaced.
For a CO2 laser, it can be used as a continuous wave and as pulsed laser with power ranging from 25 to 100 watts. By adjusting the power, exposure time (seconds), and spot size (mm), a CO2 laser can be used for incision, dissecting and vaporizing. To test the laser, use a wooden spatula.
2. Check the Environment
- Oxygen levels shall not exceed 28% in the operative field when using a CO2 laser.
- CO2 ablative lasers should never be used with nitrous oxide mask.
- Never use alcohol in the operative field and make sure the area has adequate ventilation.
3. Use Personal Protective Equipment
Everyone (patient, operator, assistant) must wear appropriate eyewear/facemasks to prevent ocular damage, and all goggles must have side shields to protect from peripheral injury and impact. Fire retardant drapes, damp packs and pads should also be used.
4. Ablate the Soft-Tissue Lesions
Small Lesions
Before beginning the laser treatment, apply topical anesthesia, administer local anesthesia, and ensure it has taken effect.
For small lesions (< 5mm diameter) ablate the lesion by spaced applications of a 3mm ablative laser beam in continuous or pulsed mode.
Large Lesions
Before beginning the laser treatment, apply topical anesthesia, administer local anesthesia, and ensure it has taken effect.
For larger lesions, use the 1 mm cutting tip on hand piece and excise the lesion. Wooden spatulas may be used to manipulate the oral tissues, but no metal instruments should be used during operation.
During the operation, suction the laser plume to remove smoke from the operating site and lessen the risk to operator and staff of inspiring vaporized blood-borne virus particles.
Bleeding is rarely a problem but in case bleeding occurs, possibly due to accessing a vessel of significant size, a combination of coagulation with the 3 mm unfocused laser beam and light pressure is effective.
Chart carefully all lesions that are treated and include the length of time the laser was applied in total, and the equipment used. Lastly, document the type, date, time of occurrence, and the date and time the laser was placed back into service to the appropriate log book.
5. Provide Post-Operative Instructions
The treated area does not require any special postoperative care; suturing, tamponade, graft cover, or dressing is unnecessary. For pain, OTC NSAIDs (e.g. ibuprofen, Advil) or acetaminophen may be taken as needed.
Do not boil, autoclave or use alcohol on laser lenses. Each lens used during a laser procedure must be washed using a solution of soap and water to clean the lens.
Especially when using Nd:YAG laser, follow-up is important because swelling and sloughing of tissue can occur at deeper planes and manifests when the superficial layers appear to have healed.
Lastly, if the patient has multiple lesions that need to be treated, the treatments should be held separately at 2-4 week intervals.
Earn a Master’s Degree in Orofacial Pain and Oral Medicine Online
Like what you’re learning? Consider enrolling in the Herman Ostrow School of Dentistry of USC’s online, competency-based 1-year certificate program or 3-year Master’s program in Orofacial Pain and Oral Medicine.
Disclaimer
The information and resources contained on this website are for informational purposes only and are not intended to assess, diagnose, or treat any medical and/or mental health disease or condition. The use of this website does not imply nor establish any type of provider-client relationship. Furthermore, the information obtained from this site should not be considered a substitute for a thorough medical and/or mental health evaluation by an appropriately credentialed and licensed professional. Commercial supporters are not involved in the content development or editorial process.