Sometimes patients will present with recurrent ulcerations of the oral cavity, and the frequency and severity are alarming. When this occurs you have to start thinking of factors that might cause these alterations.
Don’t have time to read this article? We get it. Download the Diagnosing Vesicular Ulcerative Conditions checklist to get the key information and images from this article plus all the other conditions we cover in the Dentist’s Guide to Oral Pathology.
A few factors to consider are nutritional deficiencies, blood deficiencies, and Crohn’s disease.
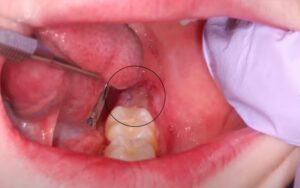
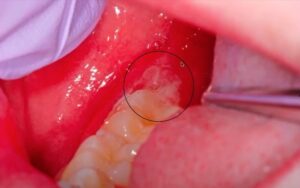
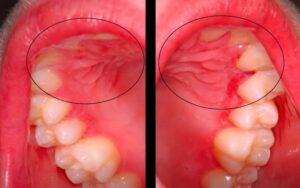
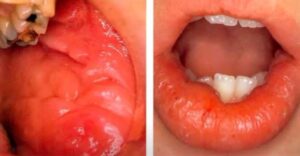
Above are some ulcerations in a patient that has Crohn’s disease. The patient’s medical history would be very important because Crohn’s can involve anywhere from the mouth to the rear end, sometimes it’s the first manifestation, the initial onset of Crohn’s disease.
The first two images above are irregular ulcerations of the left retromolar pad and the right retromolar pad from the same patient. The third image shows several gingival ulcerations. Because there is no vesicle stage at the locations, this doesn’t fit with oral herpes (Primary Herpetic Gingivostomatitis), secondary (recurrent) herpetic eruptions, or Aphthous Stomatitis.
Now we have to start thinking outside the box and ask patients clinical questions like, how are your bowel movements, have they changed, etc. If you’re not sure what it is, take a biopsy.
Biopsy of Aphthous Ulcers in a Patient with Crohn’s Disease
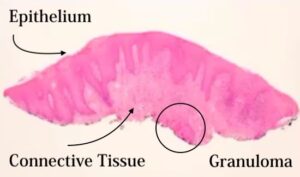
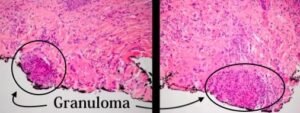
The epithelium is a little bit acanthotic in the connective tissue. It looks like there’s a little bit of inflammation, but when you go to a higher power you see these little structures. These are called granulomas.
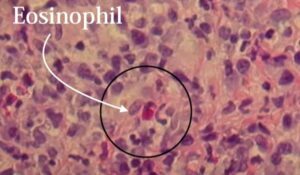
This is a granulomatous condition with eosinophils scattered throughout. Our differential for diagnosis for granulomatous inflammation would be something that’s either caused locally, or it could be a foreign material, an allergy, or a fungal infection.
We can do stains and polarize to see if any of these things show up. Not so much the allergy but the fungal or foreign material. If we do some stains for fungal and it’s negative, then we’ve got to start thinking of more systemic causes.
It can be either Crohn’s disease, sarcoid is also a granulomatous type condition, and TB. But these will be necrotic granulomas in the center.
Oral Manifestations of Crohn’s Disease
Crohn’s can manifest orally like recurrent aphthous ulcerations, but they usually are more frequent and more severe. They can also manifest orally as:
- Generalized labial mucosae enlargement
- Inflammatory hyperplasia with fissuring (cobblestone effect)
- Polypoid tag-like lesions on vestibular and retromolar mucosa
- Linear ulcerations with hyperplastic margins
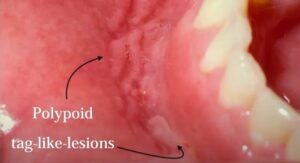
This first picture is the generalized labial enlargement and the cobblestone effect with some ring-like, tag-like lesions of the oral mucosa. The second picture shows tag-like lesions in the mandibular vestibule. It kind of looks like you punched your nail into the area. Then tag like lesions can occur which look like skin tags in the oral cavity.
Differential Diagnosis of Aphthous Ulcers
When you have aphthous ulcers that are more severe and frequent, you always want to ask if there are regions anywhere else. Behcet’s disease is something we want to think about which is ocular and genital involvement.
I had a patient once in residency and she had diffused, painful alterations. It turns out that she had an iron deficiency and her son had given her spinach for dinner one time and for a couple of days the lesions resolved after a couple of days.
Crohn’s disease colitis and then hematologic diseases as well as cyclic neutropenia, in general, can result in ulcerations at the oral cavity. These are the things one needs to think about in these patients.
Vesicular Ulcerative Conditions
Download the Diagnosing Vesicular Ulcerative Conditions checklist to get all the key information and images from this article.
Get More Information About Our Online Postgraduate Programs
Want more? Get information about our online Oral Pathology and Radiology programs for full-time, practicing dentists.

