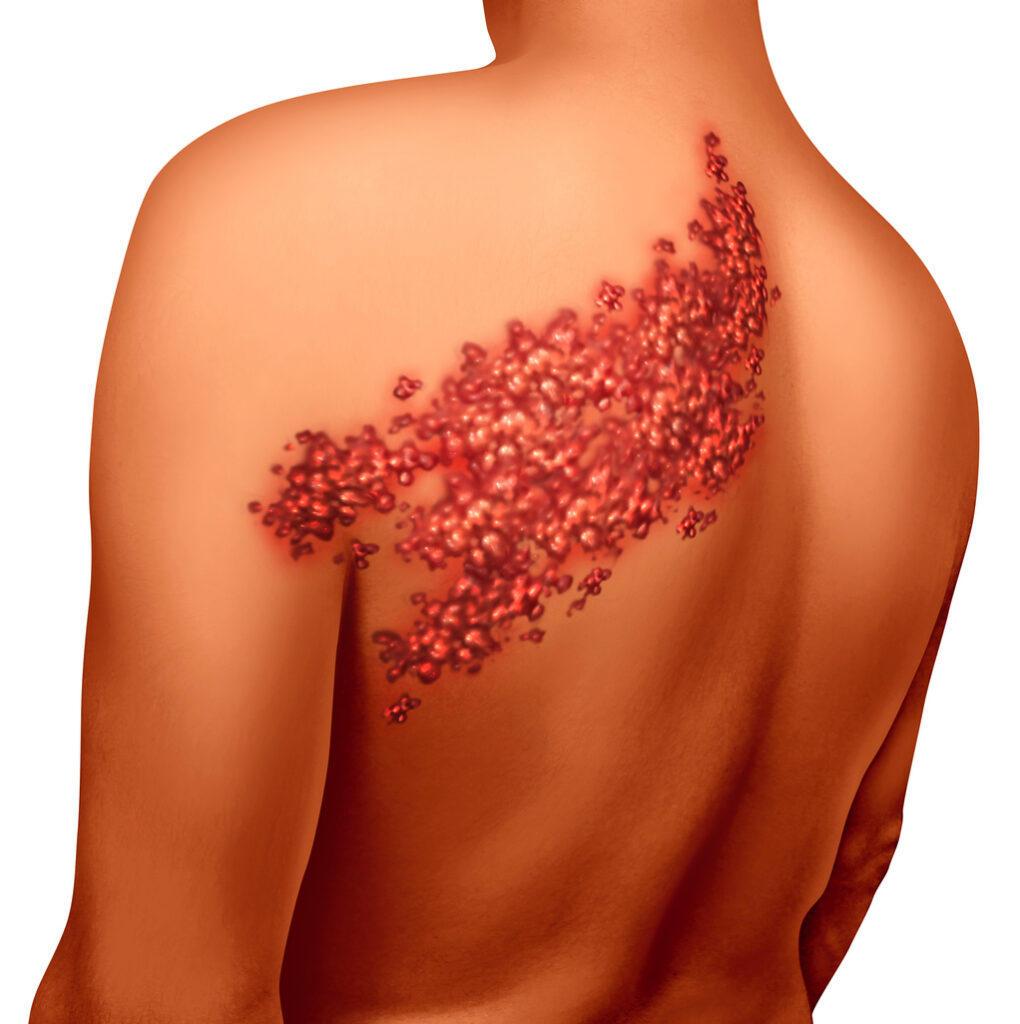
Herpes zoster is a neurocutaneous disease that is caused by the reactivation of varicella-zoster virus (VZV) from a latent infection of dorsal sensory or cranial nerve ganglia following primary infection with VZV earlier in life. (Schmader et al 2007).
- Major risk factors for HZ are age (> 65 years) and compromised immune system.
- The live attenuated zoster vaccine is effective in reducing the incidence and severity of herpes zoster and is recommended for all immunocompetent adults 60 years of age and older.
- Herpes zoster ophthalmicus (HZO) is a subtype of HZ which specifically involve the V1 distribution and can cause blindness.
- Ramzy Hunt Syndrome is a type of acute herpes zoster, which occurs by reactivation of the varicella-zoster virus at the geniculate ganglion. Clinical presentation of Ramsay Hunt syndrome includes a vesicular rash on the ear (herpes zoster oticus) or in the oral mucosa accompanied by acute peripheral facial nerve paralysis. Other cranial nerves such as V, IX, XI, and XII are often involved. (Jeon et al, 2018).
Like what you’re learning? Download a brochure for our Orofacial Pain and Oral Medicine certificate or master’s degree program in partnership with the Keck School of Medicine of USC.
In addition to general factors, such as advanced age and female gender, inflammatory rheumatic diseases and their immunosuppressive treatment are important risk factors for the occurrence of herpes zoster.
Clinical stages of VZV reactivation
- Prodrome stage (pre-herpetic neuralgia): which usually lasts for few days and is characterized by nonspecific local and general symptoms.
- Local symptoms in the affected dermatome: aching, burning, itching, paresthesia, tingling, or lancinating pain.
- General symptoms: headache, malaise, low-grade fever, and photosensitivity).
2. Acute stage (AHZ): which is marked by the eruption of skin rash in the affected dermatome and the development of VZV-induced neuritis.
- Herpetic rash: the rash is unilateral, dermatomal, red, maculopapular and usually develops vesicles and then crusting occurs followed by healing within 2-4 weeks.
- VZV-induced neuritis produces unilateral dermatomal neuralgic pain, which is described as burning, deep aching, tingling, itching, or stabbing.
3. Post-herpetic neuralgia (PHN): which is defined as pain persisting more than 3 months after the onset of the rash in the same affected area. (Hadley et al, 2016).
- Patients with PHN may experience multiple types of pain including:
— Constant pain (deep, aching, or burning pain)
— Paroxysmal pain (lancinating, stabbing, shooting)
— Hyperalgesia (an exaggerated painful response to a painful stimulus)
— Allodynia (a painful response to a non- painful stimulus).
Diagnosis of HZ
The diagnosis of HZ is mainly a clinical one and can be made with high confidence due to the characteristic clinical symptoms of this condition (unilateral, dermatomal, vesicular rash and neuralgic pain in an older patient). The initial clinical symptoms of herpes zoster are often non-specific and may lead to initial misdiagnosis.
Typically, a single dermatome is involved, although two or three adjacent dermatomes may be affected. The lesions usually do not cross the midline. Herpes zoster can also present with unique or atypical clinical manifestations, such as glioma, zoster sine herpete and bilateral herpes zoster, which can be a challenging diagnosis even for experienced physicians.
Laboratory tests: polymerase chain reaction (PCR) is used to confirm the diagnosis, especially in cases of atypical HZ presentation.
Treatments used for the different stages of VZV reactivation
Acute stage:
- Antiviral therapy: should start within 72 hours of rash onset. Antiviral therapy initiated in the first 72 h after the onset of exanthema reduces acute symptoms and the risk of complications.
- Acyclovir, famciclovir, and valacyclovir effectively treat VZV infections.
- Analgesics: can range from OTC NSAIDs to Opioids (Oxycodone) depending on the severity of pain.
- Corticosteroids: patients who were treated with corticosteroids in addition to the antivirals showed faster improvement of their symptoms. Corticosteroids are especially used for cases of VZV-induced facial paralysis and cranial polyneuritis
- Adjuvant analgesics: gabapentin or pregabalin is used in cases of moderate-to-severe herpes zoster pain which is refractory to the usual treatment.
- Anesthetic nerve blocks: used in cases of inadequate pain relief with the previous medications.
Post-herpetic neuralgia:
Pharmacological treatments: Topical lidocaine patch 5%, gabapentin, pregabalin, opioids, tricyclic antidepressants (TCAs), tramadol and topical capsaicin cream and patch. Sometimes a combination of these drugs can be used for more effective results.
Non-pharmacological treatments:
- Non-invasive treatments: cold application, TENS, PENS, psychological treatments, and acupuncture).
- Invasive treatments: peripheral and central neural blockade, central nervous system (CNS) drug delivery, spinal cord stimulation and neurosurgical techniques.
Earn an Online Postgraduate Degree in Orofacial Pain and Oral Medicine
Like what you’re learning? Consider enrolling in the Herman Ostrow School of Dentistry of USC’s online, competency-based certificate or master’s program in Orofacial Pain and Oral Medicine in partnership with the Keck School of Medicine of USC.
References:
Schmader K. Herpes zoster and postherpetic neuralgia in older adults. Clin Geriatr Med. 2007 Aug;23(3):615-32, vii-viii. doi: 10.1016/j.cger.2007.03.003. PMID: 17631237; PMCID: PMC4859150.
Hadley, G.R., Gayle, J.A., Ripoll, J., Jones, M.R., Argoff, C.E., Kaye, R.J., Kaye, A.D., 2016. Post-herpetic Neuralgia: a Review. Current Pain and Headache Reports 20. doi:10.1007/s11916-016-0548-x
Bader, M.S., 2013. Herpes Zoster: Diagnostic, Therapeutic, and Preventive Approaches. Postgraduate Medicine 125, 78–91. doi:10.3810/pgm.2013.09.2703
Jeon Y, Lee H. Ramsay Hunt syndrome. J Dent Anesth Pain Med. 2018 Dec;18(6):333-337. doi: 10.17245/jdapm.2018.18.6.333. Epub 2018 Dec 28. PMID: 30637343; PMCID: PMC6323042.
Davis AR, Sheppard J. Herpes Zoster Ophthalmicus Review and Prevention. Eye Contact Lens. 2019 Sep;45(5):286-291. doi: 10.1097/ICL.0000000000000591. PMID: 30844951.
Ehrenstein B. Diagnostik, Therapie und Prophylaxe des Herpes zoster [Diagnosis, treatment and prophylaxis of herpes zoster]. Z Rheumatol. 2020 Dec;79(10):1009-1017. German. doi: 10.1007/s00393-020-00915-y. PMID: 33141244.
Dayan RR, Peleg R. Herpes zoster – typical and atypical presentations. Postgrad Med. 2017 Aug;129(6):567-571. doi: 10.1080/00325481.2017.1335574. Epub 2017 Jun 5. PMID: 28540752.
